Everything you need to know about blood and blood plasma donation
Everything you need to know about blood and blood plasma donation
Everything you need to know about blood and blood donation
Today, there is no substitute for human blood, and blood products have a limited shelf life: as you can see, donating blood regularly is essential! Emergency care, surgical procedures, blood diseases, cancers…
Have you ever wondered: "What is blood and what is it made of?" Respiration, nutrition, defense, regulation… Blood plays an essential role in many vital functions, but what exactly is it?
Blood and its components
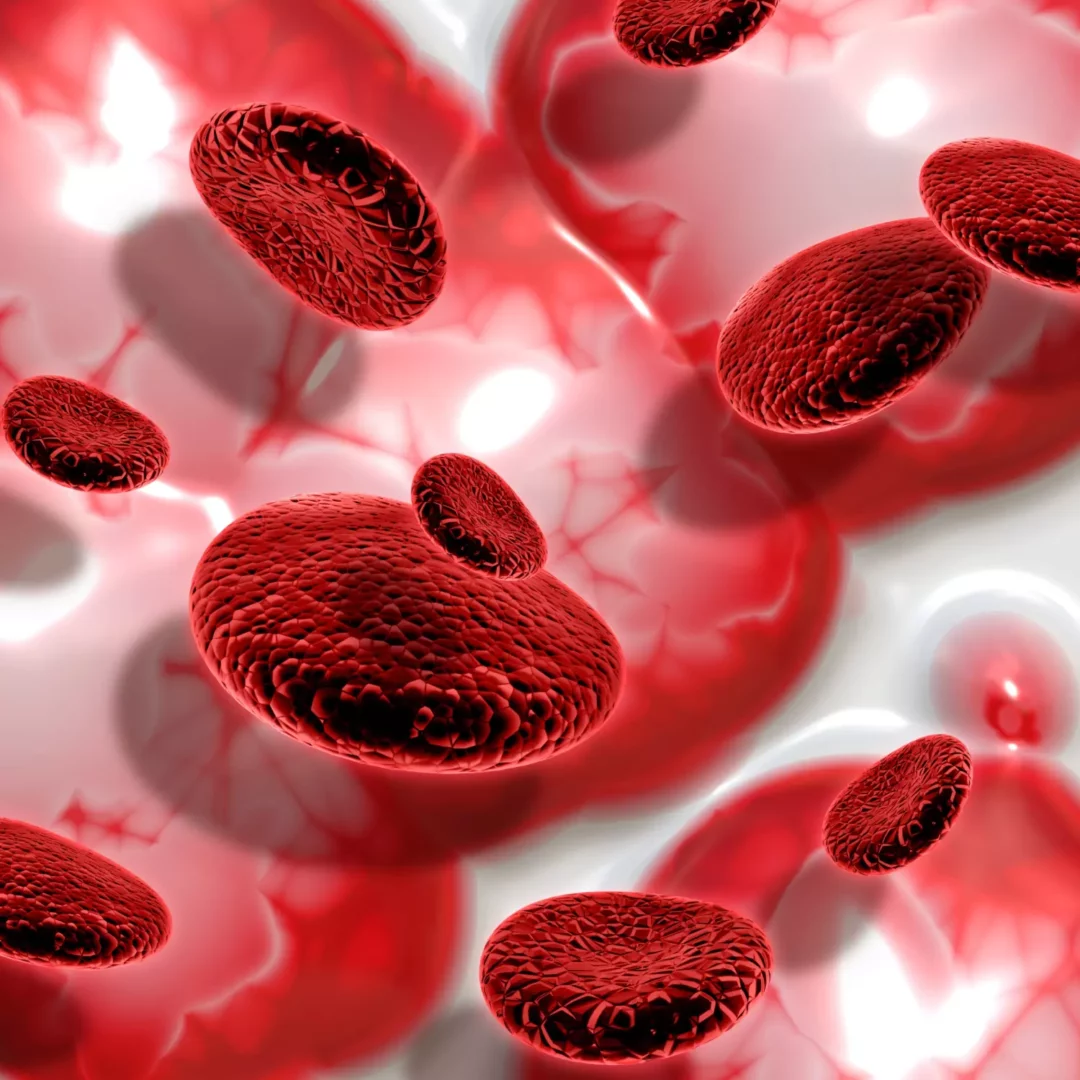
Red blood cells: the oxygen carriers
Red blood cells transport oxygen from the lungs to the tissues and, in return, collect carbon dioxide to be expelled during exhalation. Red blood cells are the most numerous cells in plasma: approximately 5 million per mm³ of blood.
Also called erythrocytes or red blood cells, red blood cells contain a protein: hemoglobin, which binds oxygen and gives our blood its red color. Their membrane is covered with proteins called antigens, which determine blood group membership: A, B, O, and AB.
A lack of red blood cells is called anemia, which causes severe fatigue. A red blood cell transfusion may be necessary in cases of severe anemia or significant bleeding.
White blood cells: the specialists of immune defense
White blood cells, also called leukocytes, protect our body against external aggressions: bacteria, viruses, parasites… There are between 4,000 and 10,000 of them per mm3 of blood!
When a pathogen invades the body, certain white blood cells detect it and form specific antibodies against it. These can be considered the body's soldiers; they fight against infections within the body.
Following a blood donation, white blood cells are filtered out: this is called leukoreduction. These cells could cause adverse effects in the recipient.
Platelets: Healing wounds and bleeding
Blood platelets are anucleate cells produced in the bone marrow. They play an essential role in blood clotting by helping to stop bleeding and preventing or halting hemorrhages. There are between 150,000 and 400,000 platelets per mm³ of blood.
When a wound is cut, these tiny cells seal the injury by adhering to the surface. Thanks to their adhesive properties, the platelets stick to each other and form a plug. Then, various plasma proteins reinforce this plug. This allows the wound to heal and forms a red scab on the surface of the wound, preventing blood loss—this is what we call coagulation.
For some patients, a platelet transfusion may be necessary to stop or prevent bleeding during certain major surgical procedures. In people with platelet deficiency or leukemia, this transfusion is vital. Other patients require it as part of chemotherapy treatment.
Platelets have a very short lifespan, only 7 days. Regular donations are therefore essential to meet the demand. Regular donations mean lives saved!
Did you know? Every day, 500 platelet donations are needed.
Plasma: the body's communication fluid
Plasma is the liquid part of blood that makes up half of the blood volume. Composed of 90% salt water, it allows red blood cells and platelets to circulate in the vascular system.
Plasma contains over a hundred proteins. Albumin, which alone makes up 60% of blood proteins, maintains fluid volume and hydration in the body. It also transports hormones and other molecules. Immunoglobulins are essential in fighting infectious agents. They help prevent and combat diseases such as tetanus, hepatitis, and rubella.
Plasma also contains clotting factors, including anti-hemophilic factors and factors that prevent thrombosis (a clot obstructing a blood vessel). A hereditary deficiency of these proteins can cause severe bleeding, as seen in hemophilia.
Plasma can be transfused or used in the form of blood-derived medications. In the first case, it is used to treat serious clotting disorders and certain rare diseases. In the second case, plasma-derived medications can treat more than a hundred diseases, such as hemophilia or primary immunodeficiency. And for some of these, they are irreplaceable because there is no alternative. Plasma-derived medications can also be used in emergency medicine, for example, in cases of severe bleeding. Make plasma donation a priority!
After your donation, the blood is never transfused directly to a patient. What happens to your blood after collection? Who is it intended for? From donor to patient, your blood donations are transformed into blood products.
In many countries, blood donation is based on ethical values: anonymity, voluntarism, non-profit status, and altruism. These values guarantee safety for you, the donors, as well as for the recipients, and the donation center is responsible for ensuring this.

Blood types
A blood type is a set of properties that classifies individuals to determine optimal compatibility during a blood transfusion. Several classifications exist, the best known being the ABO and Rh systems. There are a total of eight blood types: A+, A-, B+, B-, O+, O-, AB+, and AB-. What determines our blood type and Rh factor?
Blood types: our identity
Blood cells have an identity
Even though the composition of blood tissue is the same for everyone, the different components of blood carry individual identifying marks on their surface. These are molecules, called antigens, which vary from person to person.
Certain differences in blood cells—red blood cells, white blood cells, and platelets—and certain plasma proteins, such as immunoglobulins, define blood groups. Several dozen antigenic systems (Kell, Duffy, Kidd, etc.) are used to characterize blood cells, including more than 20 for red blood cells alone.
The most important for transfusion are the ABO and Rhesus systems, which determine blood compatibility between two individuals.
Your blood type card contains your blood identity. Like an identity card, it officially records personal data, namely your ABO blood type and Rh factor. These remain unchanged throughout your life, except possibly in the case of a bone marrow transplant.
Medical biology laboratories are authorized to issue blood type cards. Any individual, before becoming a donor, patient, or recipient, can go to one with a doctor's prescription to have their blood type determined. We can all have good reasons for wanting to know our blood type (surgery, travel abroad, sports activities, etc.).
Whatever the reason, determining your blood type is the only way to guarantee your safety during a blood transfusion. A word of advice: keep it safe with you! It could be useful.
In an accidental emergency situation, for example, knowing your blood type is crucial information if you need a transfusion.
Did you know? Due to genetic variants that can affect Rh factor, your blood must be tested twice and at different times to determine your blood type with certainty.
That's why normally your donor card is sent to you after your second blood donation!
Please note that your donor card indicates your blood type for informational purposes only. This card cannot replace a blood type card, which remains the sole reference document for any transfusion.
Blood type card: what information does it contain?
To prevent any transfusion-related accidents, your blood type card confirms your blood identity. It allows you to easily verify, if needed, whether the blood type of a donor listed on a blood bag label is compatible with yours.
Your full name and date of birth, your ABO blood type, Rh factor, and Kell blood type are recorded there. The laboratory or hospital where the tests were performed and the dates of determination are also included.
Carrying your blood type card with you at all times, like your identity card, guarantees that healthcare professionals have a quick and reliable source of information about your blood type.
Determining your blood type
When we talk about blood group, we are actually talking about the erythrocyte group, that is to say the one carried by the red blood cells.
A large number of molecules (proteins or complex sugars) are present on the surface of these globules. As some of these molecules can differ from one individual to another, they are considered antigens.
For each type of molecule possessing inter-individual variations, we speak of a system.
The best known are the ABO and Rhesus systems, but there are many others (kell, MNS, Duffy, Jk, …).
The ABO system
This is the most well-known system. It is carried by red blood cells, but also by many other cells in your body.
This system is based on a molecule which has 2 types of termination: the A antigen, and the B antigen, or an absence of termination (no A or B), designated by the O.
Some people express only A or B, others both antigens, they are then in group AB.
On the other hand, if the red blood cells do not show either the A or B antigen, the donor or the patient belongs to group O.
The Rhesus system
This is the second best-known system, at least partially.
In reality, it is based on a molecule so large that it contains several zones that can differ between individuals.
These zones are designated by the letters D, C, E, c, e.
For each of these variations, their presence is indicated by a “+” and their absence by a “-”.
The letter D corresponds to the + and – signs that everyone is familiar with. Simplistically, when there is no D antigen, the Rh factor is negative, and if it is present, the Rh factor is positive.
By combining the ABO and Rhesus systems, we obtain the eight main blood groups: A+, A-, B+, B-, AB+, AB-, O+ and O-. In France, groups A+ (38% of the population) and O+ (36%) are the most common, while groups AB- and B- are the rarest (1%).
Plasma donation by apheresis
Plasma donation is similar to whole blood donation, but the collection method is different. Using a technique called apheresis, the blood passes through a machine that retains only the plasma, then returns the other blood components to the donor. Very safe for the donor, this method allows for twice as much plasma to be collected as with a whole blood donation. And because plasma regenerates quickly, donations can be made more frequently, every six days!
Contraindications to blood donation
Permanent contraindications include active infections known to be transmissible through blood (viral hepatitis, syphilis, HIV or HTLV infection, Chagas disease, malaria); situations of exposure to undetectable transmissible agents such as prions (stays of more than one cumulative year in the United Kingdom between 1980 and 1996, growth hormone treatment before 1989, family history of prion disease, history of corneal or dura mater transplant, history of brain or eye surgery before April 2001); a history of blood transfusion or transplant, use of intravenous or intramuscular drugs, including doping substances outside a medical context, due to a potential risk of exposure to an emerging agent.
Temporary contraindications are justified by a risk of recent exposure to an infectious agent, such as a new partner or several sexual partners in the last 4 months, or an epidemic situation for agents transmissible by blood (Chikungunya, zika, dengue, etc.).
The problem of blood donation in Cameroon particularly
Despite efforts to recruit blood donors in recent years, the National Blood Transfusion Center (CNTS) is desperately short of blood bags, with only 25% of transfusion requests being met.
In 2017, 91,047 units of blood were collected, compared to 94,873 the following year, according to figures from the National Blood Transfusion Program (PNTS). In 2019, 103,359 units were collected, with a similar figure in 2020. Despite this steady increase, Cameroon is still far from meeting the national demand, estimated at nearly 400,000 units.
To address this shortfall, which represents 75% of the demand, Cameroon is placing particular emphasis on raising awareness among potential donors. This was once again the case during World Blood Donor Day.
At the same time, significant investments are underway to improve the infrastructure of blood transfusion centers, to improve access to blood donation for the Cameroonian population.
Currently, only 2% of blood donations are voluntary. The majority of donations come from the families of patients, who donate blood in order to receive a transfusion. Faced with this blood shortage, few patients receive a transfusion.
Source: toutsurlatransfusion.com
As soon as you read this article, I urge you to mobilize and make massive donations.
The Promoter.


















Comments
4